© Copyright 2005 by the Wyoming Department of Employment, Research & Planning
WYOMING LABOR FORCE TRENDS
Vol. 42 No. 5
The Structure of Wyoming Health Care Compensation
by: Douglas W. Leonard, Senior Research Analyst
The following article is adapted from Private Sector Employee Access to Health Insurance and the Potential Wyo-Care Market, a recent publication from Research & Planning on the accessibility of employer-provided health benefits in Wyoming.
Benefits are becoming a larger portion of workers’ total compensation and the rate of growth is increasing. As shown in Figure 1, wages and salaries tend to rise more slowly during periods of accelerated benefits costs (Bureau of Labor Statistics, 2004). Two such periods occurred during the early to mid-1990s and again at the turn of the century. Rapidly increasing benefit costs appear to constrain salary growth. Not only is a larger proportion of compensation dedicated to paying health care premiums but there also appear to be long-term effects on worker retirement income and employer profitability.
In order for employers to remain competitive during periods of rapidly rising costs, they may hire fewer workers or reduce benefits to current employees. “Health insurance…now costs the nation’s employers an average of $3,000 a year” (Porter, 2004).
Because the provision of health insurance is part of employers’ overall compensation plans, health insurance needs to be understood in that context. Employers’ plans and compensation strategies are, in part, a function of the economic niche occupied by their respective industries. The purpose of this article is to identify industries where intervention programs may work to reduce the number of individuals not currently covered by health insurance.
Understanding the Market: The Issues of Residency and Eligibility
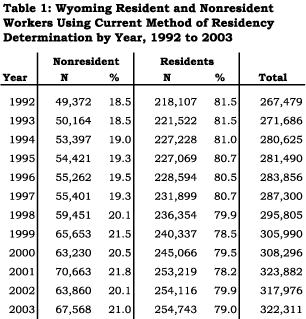
A central theme to understanding benefit access in Wyoming is residency (Jones, 2004). Residency is highly correlated with access to health insurance. Table 1 shows that the proportion of resident workers has declined steadily from 81.5 percent (218,107 workers) in 1992 to 79.0 percent in 2003 (254,743 workers). At the same time, the number of nonresident workers rose from 49,372 to 67,568. In 2003 more than one in five Wyoming workers were nonresidents. Harris (2004) estimated that on an annual average basis 9.4 percent of all UI covered workers had insufficient tenure with an employer to be eligible for health care insurance. However, nonresident workers may access health care (e.g., ER visits) while working in Wyoming. Consequently, there is a greater probability that they contribute to the cost of uncompensated care.
As shown in Figure 2, 77.5 percent of resident workers were eligible for benefits in third quarter 2002 compared to 55.5 percent of nonresident workers. Among resident workers, those who are highly tenured (five or more quarters attached to the same employer), make up three-fifths of the population (see Figure 3). The next largest group is marginal employees (those attached for short periods with long breaks) at 19.3 percent. Approximately one in ten (10.7%) resident workers were seasonal employees. Transitioning workers (9.3% of the 2002 total) are in the process of establishing a highly tenured relationship with their employer. Resident workers are more likely to maintain highly tenured relationships with employers. Therefore, they are more likely to be eligible for benefits.
Assuming that workers share at least some of the total premium cost, we see in Figure 4 that for those in the marginal or seasonal tenure categories, the average annual premium in 2002 ($2,388) is nearly equal to one quarter’s wages ($2,072 and $3,230, respectively). The ratio of annual wages to the average annual insurance cost per worker for employers is larger for those either highly tenured or transitioning status, but the average premium still constitutes a substantial proportion of total compensation.
Health insurance is also associated with firm size. The larger the firm, the greater the probability of benefits offering. Figure 5 shows that 65 percent of workers in 2002 were offered health benefits. The proportion of workers offered benefits climbs steadily from 39 percent to 56 percent as firm size increases from less than 10 employees to 49 employees, with a substantial increase to 81 percent when size increases to 50 or more employees. As shown in Table 2, more than three-quarters (75.5%) of employers in 2002 averaged less than ten workers, while only 4.1 percent employed 50 or more people.
Full-time and part-time worker status also affects the availability of health and other employer-provided benefits. The data in Figure 6 show not only the differences in benefit offerings between full- and part-time employees, but also how different benefits are made available in the workplace. Whether health, dependent health, or dental, the proportion of full-time workers offered these benefits in each case is much higher than for part-time employees.
Offering benefits to more full-time than part-time workers probably reflects employer retention strategies for employees who generate the most perceived value for their firms. Consequently, the proportions of part-time workers offered these benefits is comparatively low, with only 12 percent or one in eight part-time workers offered benefits.
Conclusion
An estimated 34,832 full-time and 49,018 part-time workers were not offered health benefits in 2002 (Gallagher et al., 2005). Because firm size and compensation are correlated, the 2,301 firms with an average size of 10-19 employees, and the 1,438 firms with 20-49 employees (see Table 2) in low-turnover industries may prove to be the most promising candidates for a health care coverage intervention program. At 17.4 percent, Manufacturing’s turnover rate is below the state average of 24.8 percent. Lower turnover levels also characterize Wholesale Trade, Financial Activities, and Education & Health Care. The starting point for an insurance initiative could be the almost 16,000 workers not offered health insurance in these industries.
Two other industries strongly suited to a health care coverage program are the expanding industries of Leisure & Hospitality and Retail Trade (Leonard, 2003). As shown in Table 3, part-time employment makes up nearly half (46.6%) of Leisure & Hospitality’s workforce and over one-quarter (27.3%) of Retail Trade’s. Leisure & Hospitality and Retail Trade comprise 18.4 and 15.8 percent, respectively, of total employment. Given the size of these industries, their projected growth, and their large share of part-time workers, employees in these industries are ideal candidates for insurance coverage programs.
References
Bureau of Labor Statistics. (2004, July 29). Employment cost index. National compensation survey. Retrieved August 23, 2004, from http://www.bls.gov/ncs/ect/home.htm
Gallagher, T., Harris, M., Hiatt, M., Leonard, D., Saulcy, S., & Shinkle, K. R. (2005, February). Private sector employee access to health insurance and the potential Wyo-Care market. Casper, WY: Wyoming Department of Employment, Research & Planning.
Harris, M. (2004, June). Industry variation in the percent of jobs with insufficient work tenure to qualify for health benefits. Wyoming Labor Force Trends. Retrieved August 23, 2004, from http://doe.state.wy.us/LMI/0604/a2.htm
Jones, S. (2004, August). Worker residency determination - Wyoming stepwise procedure. Retrieved August 27, 2004, from http://doe.state.wy.us/LMI/0804/a1supp.htm
Leonard, D. (2003). Table 2.1: Wyoming statewide employment forecasts, 1990-2010. In Gallagher, T., Harris, M., Leonard, D., Liu, W., & McVeigh, B. (2003, April). Employment Outlook: 2010 (chap. 2, p. 7). Retrieved August 23, 2004, from http://doe.state.wy.us/LMI/EmpOutlook2010.pdf
Porter, E. (2004, August 19). Rising cost of health benefits cited as factor in slump of jobs. The New York Times. Retrieved August 23, 2004, from http://www.nytimes.com/2004/08/19/business/19care.html?th
Table of Contents | Labor Market Information | Wyoming Job Network | Send Us Mail
These pages
designed by Julie Barnish.
Last modified on
by Susan J. Murray.